Opioid free anaesthesia humeral condylar fracture bupivacaïne ovh cat
DOULEUR CHEZ LES CHIENS ET CHATS
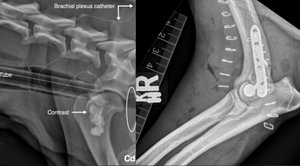
1/ Opioid-free anaesthesia (OFA) in a springer spaniel sustaining a lateral humeral condylar fracture undergoing surgical repair
Geddes, AT., Stathopoulou, T., Viscasillas, J., Lafuente, P.
Veterinary Record Case Reports, 2019, 7: e000681.
Résumé :
A two-year, three-month-old male entire springer spaniel presented for right thoracic limb lameness. Radiographs of both elbows revealed a right lateral humeral condylar fracture. Local anaesthesia using bupivacaine was supplied to the site using a continuous stay peri-neural catheter at the brachial plexus. The fracture was stabilised using a lag screw and locking compression plate (LCP) plate. No response to surgical stimulation was noted on the patient’s vital parameters during anaesthesia, systemic analgesia was deemed not to be required. Bupivacaine was administered through the brachial plexus catheter every seven hours postoperatively. Pain scores were noted to be low, hence no systemic opioids were provided. The use of a continuous peripheral nerve block allowed for cold packs and passive range of motion exercises the same day of surgery. It also allowed for a lack of requirement of systemic opioids for the duration of hospitalisation.
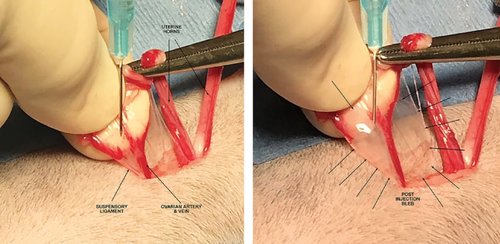
2/ Evaluation of targeted bupivacaine for reducing acute postoperative pain in cats undergoing routine ovariohysterectomy
Fudge JM, Page B, Mackrell A, Lee I.
J Feline Med Surg, 2019 Feb 5
Résumé :
This study sought to determine if bupivacaine targeted at specific, potentially painful sites could enhance postoperative analgesia in routine feline ovariohysterectomies. A secondary objective was to assess the utility of multiple acute pain scales for cats in a high-volume surgery setting. Methods: Two hundred and twelve cats were included in a prospective, randomized, double-blinded, placebo-controlled clinical trial. Anesthesia included buprenorphine, ketamine, dexmedetomidine and isoflurane. A ventral midline ovariohysterectomy was performed and cats were administered bupivacaine (2 mg/kg), placebo control (0.9% saline) or sham control (observation only) intraoperatively at the ovarian suspensory ligaments and vessels, uterine body and incisional subcutaneous tissues. Two pain scales were used to assess cats postoperatively. Initially, a multidimensional composite pain scale (MCPS) and a 0–10 numeric pain rating scale (NRS) were used. Subsequently, the MCPS was replaced with a modified Colorado State University Feline Acute Pain Scale (mCSU). Pain scores for the test groups were compared using a one-way ANOVA and a Holm–Bonferroni post hoc analysis when a difference was found (P <0.05). Results: Pain for the bupivacaine group was lower than the control groups at 1 h post-recovery and discharge, attaining significance with higher body weights. The P values were 0.008 and 0.004 for 1 h post-recovery and discharge, respectively. Pain scores between evaluators for the MCPS and NRS correlated poorly with r values for 1 h post-recovery and discharge of −0.08 and 0.22, respectively. Additionally, the MCPS proved difficult to use and time consuming, especially for feral and fractious patients, and was replaced with the mCSU. Conclusions and relevance: Targeted bupivacaine reduced early postoperative pain scores following routine feline ovariohysterectomies. The technique used was simple, requiring just over a minute to perform at minimal additional cost. The MCPS was not ideal for use in a high-volume spay setting.